AI for seniors is emerging as one of the most meaningful applications of technology. Not because it prolongs survival, but because it protects independence. For older adults, autonomy is often the difference between living and being sustained. AI is entering that space with precision and humility.
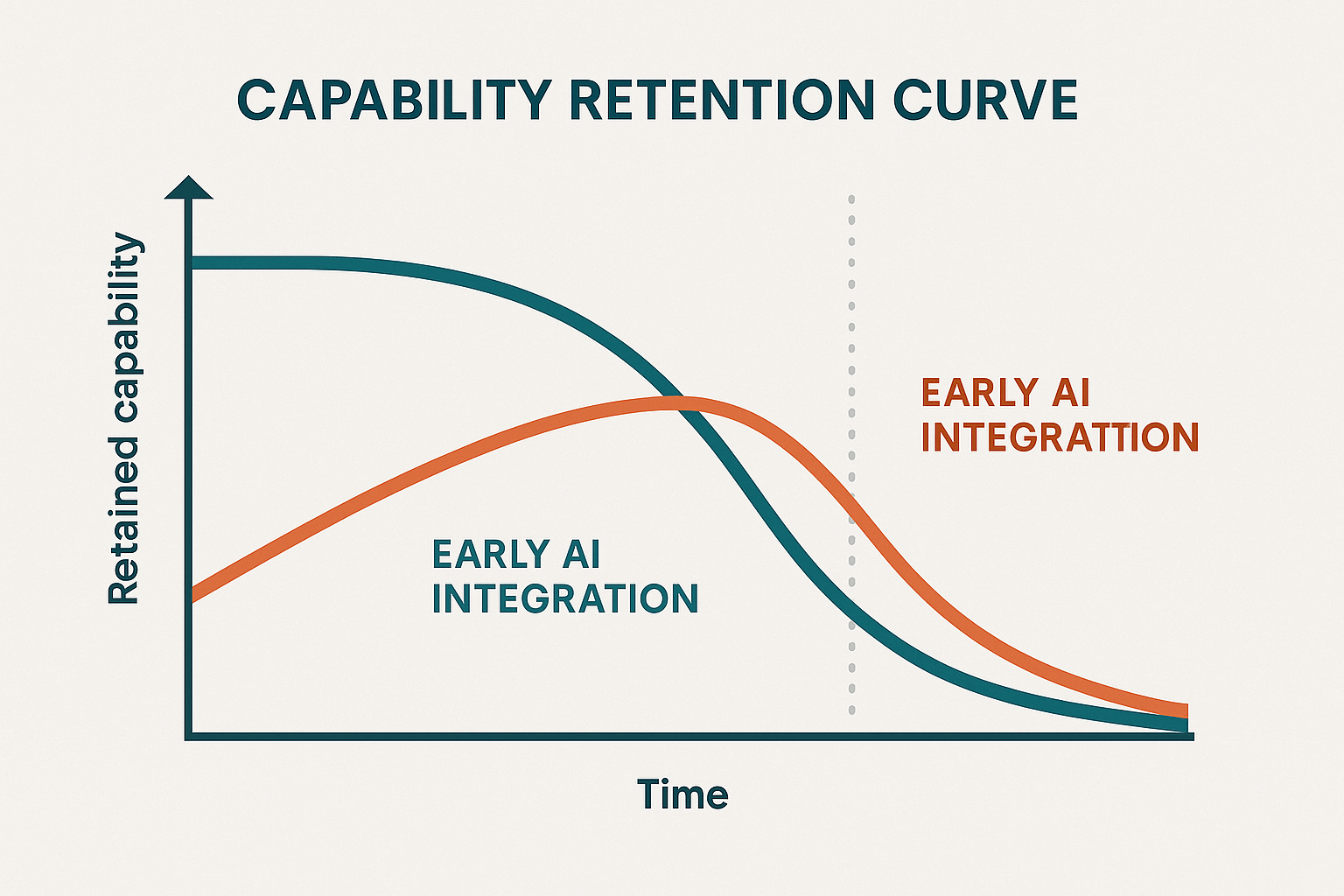
AI for seniors is particularly powerful when introduced before functional decline sets in.Devices that checkpoint mobility. Assistants who remember medication even when their memory starts to slip. Predictive systems that detect decline before symptoms surface. These are not futuristic concepts. They are products already in use throughout Europe, the US, Asia and increasingly across Africa.
The question is no longer whether AI can provide care. It is whether we will deploy it early enough to protect the capability rather than commemorate it.
Why AI for seniors matters now
The world’s ageing population is growing faster than most care infrastructures can cope with. The World Health Organisation estimates that one in six people globally will be over sixty by 2030.
By 2050, the number of people aged 80 and above is expected to triple. No health system is fully prepared for that. Developed regions face rising costs and a shortage of caregivers. Emerging regions struggle with underfunded care structures that often intervene only once decline becomes irreversible.
AI enables a shift from reactive to preventive care. It monitors patterns in activity, voice, and engagement. It signals when something changes before symptoms emerge. That single shift turns time into the core health resource.
Three functional layers of AI in senior care

1. Daily maintenance
AI supports routine before an interruption occurs. Smart pill dispensers track missed doses. Assistants like Alexa Together and Google Home Hub offer reminders, hydration alerts and conversational troubleshooting.
Where the internet is limited, SMS-based reminders or USSD-triggered check-ins are being tested in Senegal and parts of Ghana through community health programs.
For seniors who are still living independently, this layer serves as a silent reinforcement.
2. Health monitoring and prediction
The true promise of AI for seniors lies in its ability to detect micro-deviations early. Wearable technology and at-home sensors monitor patterns in posture, heart rhythm, stepping speed and sleep consistency. Solutions from Biofourmis, SenseAi and CarePredict can identify deterioration up to 72 hours before the first observable symptom.
A recent study in Nature Ageing found that AI systems identified mild cognitive impairment 6 months earlier than a typical medical assessment.
In regions where wearable deployment is limited by cost, lower-bandwidth systems are being adapted for smartphone-based gait monitoring.
A pilot program in Eldoret, Kenya, trained AI models to detect balance shifts using body movement captured by mobile cameras.
3. Emotional and cognitive support
Loneliness accelerates ageing. AI conversational tools do not provide replacement companionship, but they offer stabilisation.
ElliQ, an AI companion deployed in selected US care programs, demonstrated a 30 per cent increase in daily engagement during the first 90 days.
In Japan, a pilot use of AI-guided conversational agents with elderly people living alone showed measurable reductions in anxiety and agitation markers among dementia patients.
Apps like Replika and Woebot, when used under supervision, can provide a sense of mental continuity. They evaluate tone and sentiment and respond with corrections or prompts. They do not attempt human empathy. They maintain awareness.
Real implementation examples
One Lagos-based case involved a 73-year-old retired engineer using a solar-powered health-monitoring unit connected to his smartphone. AI detected a reduction in walk distance and a decline in hand precision. Medical consultation led to an early Parkinson’s diagnosis.
Treatment began months earlier than a typical symptom-driven consultation. Tech costs averaged $12 a month and were entirely for mobile data.
A contrasting case in rural Zimbabwe used a basic motion-sensor network connected via a solar Wi-Fi relay. A local community nurse was notified when movement became irregular. Intervention prevented a fall-induced broken hip, which would have required weeks of clinic stay across district boundaries.
In emerging regions, AI for seniors could be the only scalable alternative to physical in-person evaluation.
Interface design: critical but overlooked
Senior care AI fails when screens are complex. Adaptation should favour voice controls, high-contrast visual modes and reduced touch requirements for those with tremors or visual degradation.
Microsoft’s research division found that voice-first AI assistants were adopted at an 86 per cent success rate among first-time elderly users compared to 42 per cent with app-style tap interfaces.
The interface should adapt to the user, not expect the user to adjust to the interface.
Family integration as a fourth layer
AI’s most effective configuration combines professional, AI-driven and family-based decision loops. Family members receive alerts only when early deviation is detected.
They do not act as constant observers, but as intentional safety nodes. This framework reduces caregiver fatigue and makes the elderly feel monitored with discretion rather than intrusion.
Providers like GrandPad and Birdie now allow controlled visibility rights so relatives can view health indicators without overwhelming detail.
Implementation Guide
| Step | Action |
|---|---|
| Introduce while independence remains | Trust forms before reliance |
| Use minimal-interaction tools | One-touch or voice first |
| Configure alert thresholds | Only escalate when deviation exceeds known limits |
| Adapt for mobility/vision constraints | Test interface with real seniors |
| Keep AI in monitoring role | Human interprets, AI observes |
Regulatory outlook
The EU AI Act categorises healthcare AI as high-risk and requires visibility into decision logic.
US FDA guidance is shifting toward adaptive AI models with defined override hierarchies. Kenya and Rwanda are drafting data protection standards that incidentally apply to AI-assisted health frameworks.
Future regulation will require transparent advisory roles, correct classification and verification systems. Selecting vendors that already comply with international health data protections reduces future legal exposure.
Longevity optimisation: future direction
Longevity-based AI systems are progressing beyond monitoring. Labs such as Altos, DeepMind and Insilico Medicine are developing real-time biological feedback loops.
These could soon generate lifestyle optimisation plans such as exercise cadence, sleep rhythm, and micronutrient timing based on digital biomarkers.
We are likely three to five years away from AI systems prescribing adaptive living strategies that proactively extend functionality rather than monitor decline.
Ten-year projection
By 2035:
- AI health data will be mandatory in senior care planning.
- The age of transition into full-care facilities may shift from 74 to 78.
- AI-assisted cognitive training will become standard before the onset of Alzheimer’s.
- Community caregivers will rely on AI to triage early-risk cases in resource-constrained regions.
Change begins at home, not at the hospital.
AI for seniors aligns with the broader shift towards predictive systems, as we explored in How AI Is Redesigning the Financial Operating System of Business.
Final call
AI for seniors is not a rescue technology. It is a preservation system. Its real value appears not when decline is obvious, but when function is still intact and worth protecting. Waiting until care feels necessary turns AI into a monitoring tool. Introducing it earlier makes it an autonomy tool.
The turning point is simple: AI is most effective when it blends into daily life. That moment, when it feels almost unnecessary, is exactly when it is doing its best work.
What AI ultimately offers is not just support. It offers time, the time to remain capable, time to remain independent, time to remain oneself.

